ABCDE’s
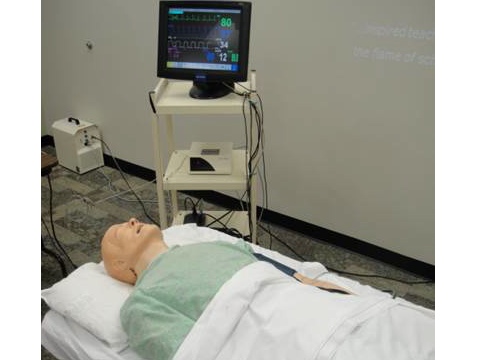
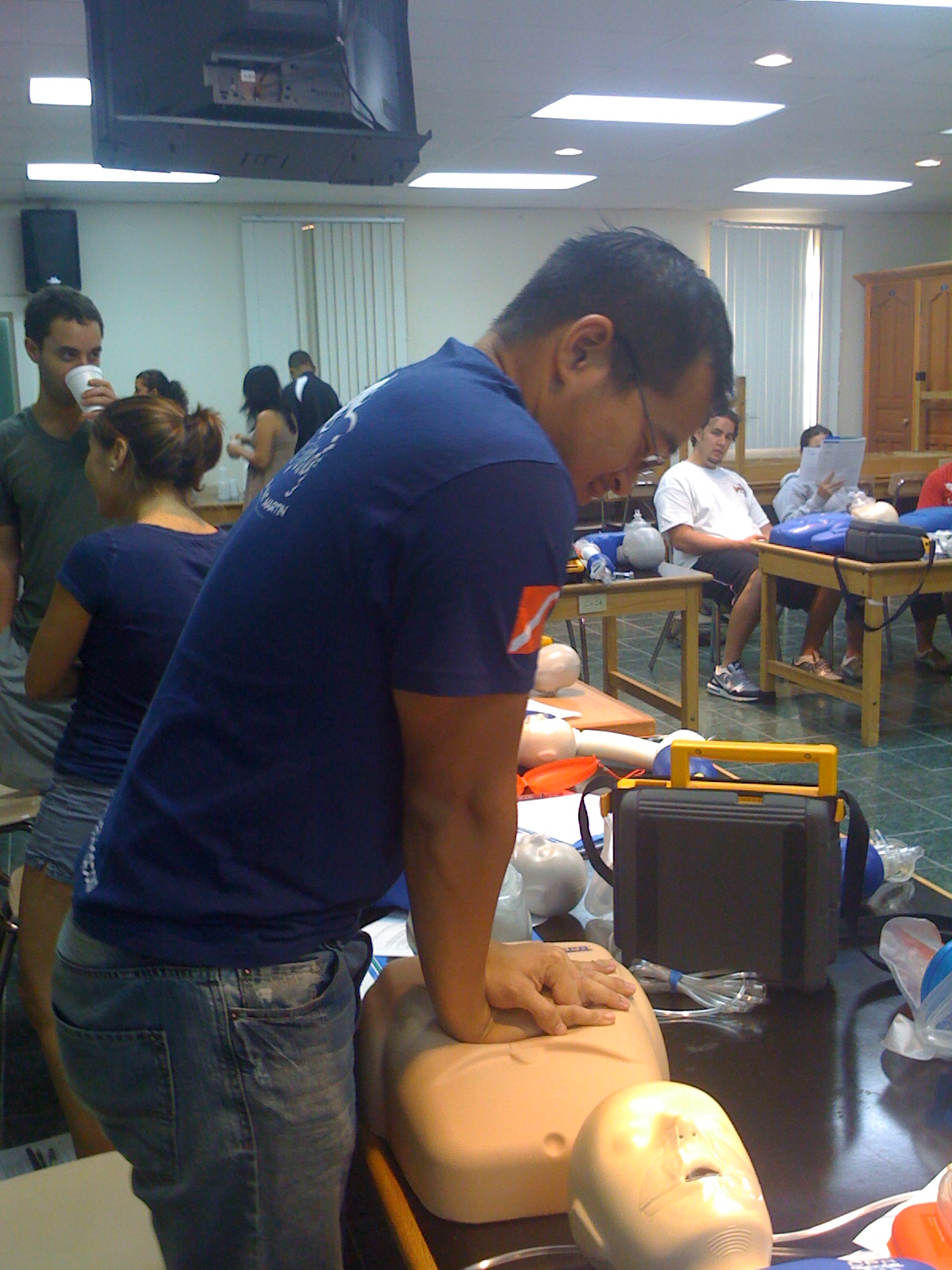
Earlier this week, two of my AUC colleagues and I had an awesome Sim Man learning session together with Dr. Butler. This is the first of two Sim Man sessions that I am required to attend for my rotation at the Royal Blackburn Hospital. I thought the session was very helpful and Dr. Butler did a great job preparing the four different scenarios we saw of varying severity. Compared with my first Sim Man experience on the island, I thought my team and I were much more confident this time in taking immediate action and working together to stabilize our patient, ordering the relevant blood tests, and determining the cause of the emergency.
- Go into room, see patient.
- See if the patient is conscious. Ask the patient if he can hear you.
- Simultaneously, have someone hook up an O2 saturation meter, ECG, and blood pressure cuff, and monitor the stats of the patient.
- Airway (A) — First, check the airways, and see if you can feel for air coming out of the mouth or nose. See if there is anything blocking the mouth or throat. Listen for any verbal response, stridor, snoring, or gurgling. If the patient is talking, then it’s a good indication that the patient does not have any emergency problems with his/her airway or breathing. If there is snoring, then the soft palate or tongue is probably blocking the airways. If you see the airway is impeded, then put in a tube. Put on an O2 mask to bring up a low O2 saturation (i.e. if the saturation is below 92%).
- Breathing (B) — Look for cyanosis, check for respiratory rate, and look at the chest movement to see if the patient is breathing. For chest movement, take note if it is bilateral or unilateral, or paradoxical. Sometimes the airway may be open, but the patient may not be breathing. If this is the case, then you must do artificial breathing.
- Circulation (C) — While one of your team members is checking the airway and breathing, do not hesitate to have another person immediately check for pulse, to see if it is full, weak, or absent. If there is no pulse then immediately perform CPR (i.e. 30 pumps to 2 breaths). In one of our Sim Man scenarios, we walked into the room to find our patient already in cardiac arrest, and the way we could figure this out immediately is by figuring out he did not respond to our voice, or pinches, was not breathing, and did not have a pulse. Two of us immediately went into CPR while the other hooked up the monitors to the patient. It took us about 3 rounds to revive him. Had we have waited on checking the pulse or initiating CPR, the patient may not have survived. Other things to look for in circulation: Feel the temperature and notice the colors of the extremities. If it is cold and blue, then there’s a lack of circulation. Look at urine output, blood pressure, check to see if there are heart sounds and feel for pulse! Check capillary refill time by pressing down on the patients skin, and then see how long it takes for the finger to return from white to pink. If it takes longer than 2 seconds, then there is poor circulation. If the blood pressure falls to a critical level, then give IV fluids. Before giving the fluids, however, extract the blood you need for doing a complete blood count, LFTs, or any other blood assays you feel you must order for the patient, given the history. It’s important to extract the blood you need first before giving IV fluids, otherwise you may not have an accurate reading with the blood once it’s dilated with the IV fluids.
- Disability (D) — Remember the mnemonic “AVPU,” which stands for Alert/Voice/Pain/Unresponsive. Basically check to see if the patient is alert, or if the patient is not alert, is he responsive to voice? If not to voice, is he responsive to pain (pinch the patient, or rub his sternum with your knuckles to see if he responds). If neither of these techniques can alert him, then the patient is unresponsive. Also, check the pupils and check for pupillary light reflex! Because my team and I checked one of our Sim Man’s pupils, we discovered that his eyes was pin-point, and given the history, determined that the patient entered a state of emergency from the morphine he was given for his surgery. Another important thing to check is the glucose in the blood, as low blood sugar may be the source of emergency. You can get the glucose checked from the blood you withdrew from the previous step.
- Exposure (E) — Don’t underestimate the importance of visual inspection! Often times, simply checking the patient’s body will reveal the source of the emergency. In one of our Sim Man scenarios, my team and I only discovered the source of low blood pressure in our patient by lifting up his gown to discover bleeding at the site of a surgical wound, as well as excessive blood in the surgical drainage. This patient was in hypovolemic shock! Learning from this, make sure to look at the whole body, from the abdomen, to the legs and genitalia.
So those are the ABCDE’s of immediate assessment in emergency situations. After two years of learning medicine by sitting in lecture and taking exams, we as students (or at least I do) develop a tendency to start immediately figuring out the diagnosis, rather than figuring out first how to stabilize the patient. But if there is one take-home message to this Sim Man session, it is to stabilize the patient first before anything else. Once the patient is stabilized and is away from any harm or risk of cardiac arrest, then we can have more time to make a definitive diagnosis, and further treat or refer accordingly.