Female Reproductive Endocrinology in 28 Easy Steps
 In my med school experience, Female Reproductive Endocrinology is one of the more challenging things to learn in physiology, since hormones rise and fall, and interact with each other in different ways in different phases of the cycle. But when broken down to 28 steps, the process is easier to understand.
In my med school experience, Female Reproductive Endocrinology is one of the more challenging things to learn in physiology, since hormones rise and fall, and interact with each other in different ways in different phases of the cycle. But when broken down to 28 steps, the process is easier to understand.
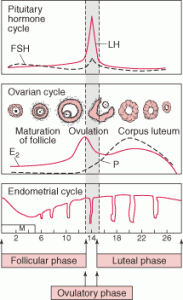
- Menstruation marks the beginning of the menstrual cycle, because you can see it easily. First day of cycle = first day of bleeding.
- The menstrual cycle begins with the Follicular Phase, followed by ovulation, and then the Luteal Phase. The first phase, Follicular Phase, lasts for about 2 weeks but can vary depending on the individual. In contrast, Luteal phase is always 14 days.
- During the Follicular Phase, estrogen is made predominantly, which causes thickening of the cell lining in the endometrium.
- In contrast, during Luteal Phase, progesterone is predominant hormone made, which causes thick secretions in the endometrium. Both the thickening in the cell lining and secretion of thick mucus in the endometrium are needed for the ovum to implant in the uterus.
- Menses is not active phenomena. Unless you implant ovum, make trophoblast, and secrete hCG, corpus luteum will wither away. No corpus luteum means no estrogen and no progesterone made, which means no maintenance of cells lining or secretions in endometrium, which leads to the sloughing of endometrial layer from the uterus, causing menses.
- In the ovarian follicle, there are two types of cells: Granulosa cells and Theca cells. The Theca cells have LH receptors and are therefore stimulated by Luteinizing Hormone (LH) while the Granulosa cells have FSH receptors (or at least during this phase) and are stimulated by Follicular-stimulating hormone (FSH).
- Theca cells form the outer-most layer of the follicle, while Granulosa cell layer form the second layer. Being the outer-most layer lets the Theca cells uptake LDL cholesterol from the bloodstream, which it converts to pregnenolone, then to androgens (Androstenedione and DHEA) with Desmolase, after stimulation by LH (which increase cAMP in theca cells). The androgens produced are then passed to the Granulosa cell layer below, which converts the androgens to estrogen via Aromatase, after stimulation by FSH (which increase cAMP in granulosa cells). The estrogen produced then goes toward the center of the primary oocyte, then surrounds the egg in the center of the follicle.
- While most of the estrogen made stays inside the egg to proliferate the granulosa cells, some of the estrogen (and inhibin) made by the Granulosa Cells during the Follicular phase goes into the bloodstream and causes feedback inhibition of FSH and LH production in the pituitary. FSH is inhibited more than LH. The fall in FSH causes only dominant follicle survive, but that one follicle will get all the FSH available and continue to increase its FSH receptors and be maintained. You only want 1 dominant follicle to survive because ideally you only want 1 baby at a time, rather than 20 or 100 babies. Also, you’re only born with a set number of eggs, and you don’t want to waste them (Born with 1,000,000 eggs but drops to 400,000 during puberty).
- Estrogen is inhibitory on FSH ONLY DURING BEGINNING PART OF FOLLICULAR PHASE!!!
- Estrogen stimulates the development of female accessory organs, secondary sex characteristics, causes endometrial cells to grow, and causes cervical mucus to be thin and watery, making it easy for sperm to go through the cervix. Remember the sperm has to get to the egg by Day 15 of menstrual cycle so that the egg can reach uterus by Day 20 and implant and make beta-hCG by Day 25. You need to have watery, thin mucus for sperm to do this (vs. thick, viscous mucus).
- IMPORTANT: In the initial part of the Follicular Phase, estrogen is inhibitory for FSH at low levels. But later on when estrogen level increases to a certain threshold, estrogen switches from being inhibitory to being stimulatory, and now you have a positive feedback loop. This is one of the few places in the body (along with oxytocin) where you see positive feedback.
- Estrogen stimulates FSH and LH production, FSH/LH makes estrogen, and so forth until you have a huge surge in both FSH and LH. Although both FSH and LH surge, only LH surge needed for ovulation. Ovulation occurs only after the estrogen peaks. If estrogen levels are still rising, ovulation hasn’t occurred.
- You then Ovulate! The egg comes out of the follicle, and the fallopian tube flaps its fimbriae to create a current that would bring the egg into its lumen.
- The egg-less follicle after ovulation is now called the Corpus luteum. It remains in the ovary and is named after its yellow, fatty appearance. This marks the beginning of the Luteal Phase. Unlike the Follicular Phase, it now produces predominantly Progesterone, and just a little bit of estrogen. As said above, the Corpus luteum lasts exactly 14 days, and passively expires after those 14 days unless it is “rescued” by hCG from placenta if fertilization and implantation occurs. Therefore, the day you menstruate minus 14 days = the day you ovulated.
- IMPORTANT: The rise in FSH and E2 rise causes LH receptors to form on Granulosa cells (remember LH receptors were previously only found on Theca cells). Like Theca cells, LH signal now also causes these “luteinized” Granulosa cells to convert cholesterol into pregnenolone, which converts to progesterone, the predominant hormone produced during the Luteal Phase by the corpus luteum. Side Note: Although both Granulosa and Theca cells are now luteinized, only Granulosa cells have aromatase and make estrogen. The aromatase inhibitors (Anastrazole, Lanosterol, Exemestane) work here. Side note: The only places in the body where estrogen is made are granulosa cells and adipose tissue. Obese men are more likely to have gynecomastia not merely because they have more fat around that area but also because more adipose tissue means more estrogen.
- Progesterone causes the endometrium to become secretory to provide nutrients for the trophoblast. It also makes cervical mucus thick, to prevent sperm and bacteria to the growing blastocyst/fetus. Progesterone also temporarily raises the woman’s basal body temperature (BBT). By the time you notice an increase in your body temperature, most likely you have already ovulated, and whatever egg you fertilize now will unlikely make it in time for it to be viable.
- Corpus luteum makes progesterone (and some estrogen) for the next 14 days, maintaining endometrial lining, a good environment for implantation. However, the progesterone levels decreases throughout those 14 days because progesterone has feedback inhibition on pituitary, causing a decrease in LH (and FSH) production, and therefore decrease in progesterone (due to decrease in LH). Without LH-signal for progesterone (and some estrogen) production, the corpus luteum withers away.
- If the ovum is fertilized with a sperm, the zygote will implant in the endometrium, become a trophoblast, and make beta-hCG, which will “rescue” the corpus luteum from its original short 14-day lifespan. Beta-hCG has a beta subunit that resembles LH, which stimulates the corpus luteum to continue producing progesterone, maintaining the pregnancy.
- From the start of the Luteal Phase, you have only 14 days to fertilize (takes 8-25 hours), implant (takes six days), make trophoblast, and make beta-hCG (takes 11 days, which you can detect w/ pregnancy tests). You only have 14 days to do all of these before the corpus luteum disintegrates. If you delay any of these steps, namely fertilization, for 2-3 days even, you won’t finish all of these steps in time for corpus luteum to survive. You could still fertilize an egg, but if that zygote doesn’t make it in time to the endometrium to get implanted, and waits only until after the corpus luteum have disintegrated to produce beta-hCG to maintain the corpus luteum, then the zygote won’t survive because there is no corpus luteum there to produce progesterone to maintain the pregnancy (unless you artificially inject progesterone into yourself). The endometrium therefore can’t be maintained, and sloughs off, causing bleeding, aka menstruation.
- The trophoblast must depend on the corpus luteum for progesterone and estrogen throughout the first trimester of pregnancy, after which it can start making its own progesterone and estrogen.
- Second 2/3 of pregnancy, placenta is developed enough to produce its own progesterone. If you need to remove ovaries, you should remove it after first trimester because by this time the placenta is developed enough to make it’s own progesterone to maintain itself, and you no longer need the ovaries’ help to maintain the pregnancy.
- Placenta brings in LDL to make progesterone. DHEA-S (sulfated DHEA, must be sulfated to get across placenta to make lipid-soluble (all steroid hormones are lipid-soluble except DHEA)) from fetal adrenal cortex is also converted by aromatase in the placenta to make extra estrogen for the mother.
- All that extra estrogen helps mother grow the uterus, and helps make prolactin, which grow the breasts. But at the same time it prevents milk synthesis, since the baby hasn’t been born yet.
- Human placental lactogen (HPL) (“anti-insulin” in mother, like growth hormone) is also released. HPL causes whatever glucose is available to go to the baby if the mother starves. HPL is one of the reasons for gestational diabetes, which may occur in patients who had a genetic predisposition to diabetes. During gestational diabetes, the mother gets free fatty acid and ketones while the fetus gets the sugar.
- Pregnancy also resets the osmolarity sensor in the hypothalamus, so that you continue making ADH, even if your blood osmolarity is low. This leads to higher cardiac output to support circulation of both baby and mother.
- Estrogen also increases oxytocin receptors in myometrium. Oxytocin functions in uterine contraction during labor as well as milk ejection during breastfeeding.
- During labor, hypothalamus releases oxytocin, which helps uterus contract. Despite its role in uterine contraction, oxytocin isn’t what triggers it. The trigger is currently unknown. If for some reason you don’t have oxytocin, you can still give birth. It is not considered essential and there is no disease from too much oxytocin.
- Estrogen levels decrease after parturition (delivery), meaning milk is no longer prevented from flowing. Suckling stimulates brain to inhibits Dopamine (which also acts as prolactin-inhibiting hormone) and GnRH production. Inhibition of Dopamine increases prolactin, stimulating the production of milk. Inhibition of GnRH prevents LH surge and therefore prevents ovulation so you don’t get pregnant while still breastfeeding your child. Suckling also triggers oxytocin release from hypothalamus, causing myoepithelial cells contraction in the breast, ejecting the milk. A dose of estrogen will stop the milk from flowing again.










Thank you for this! makes so much more sense 🙂
Glad this helped Rebecca!
Thank you, that helped a lot 🙂